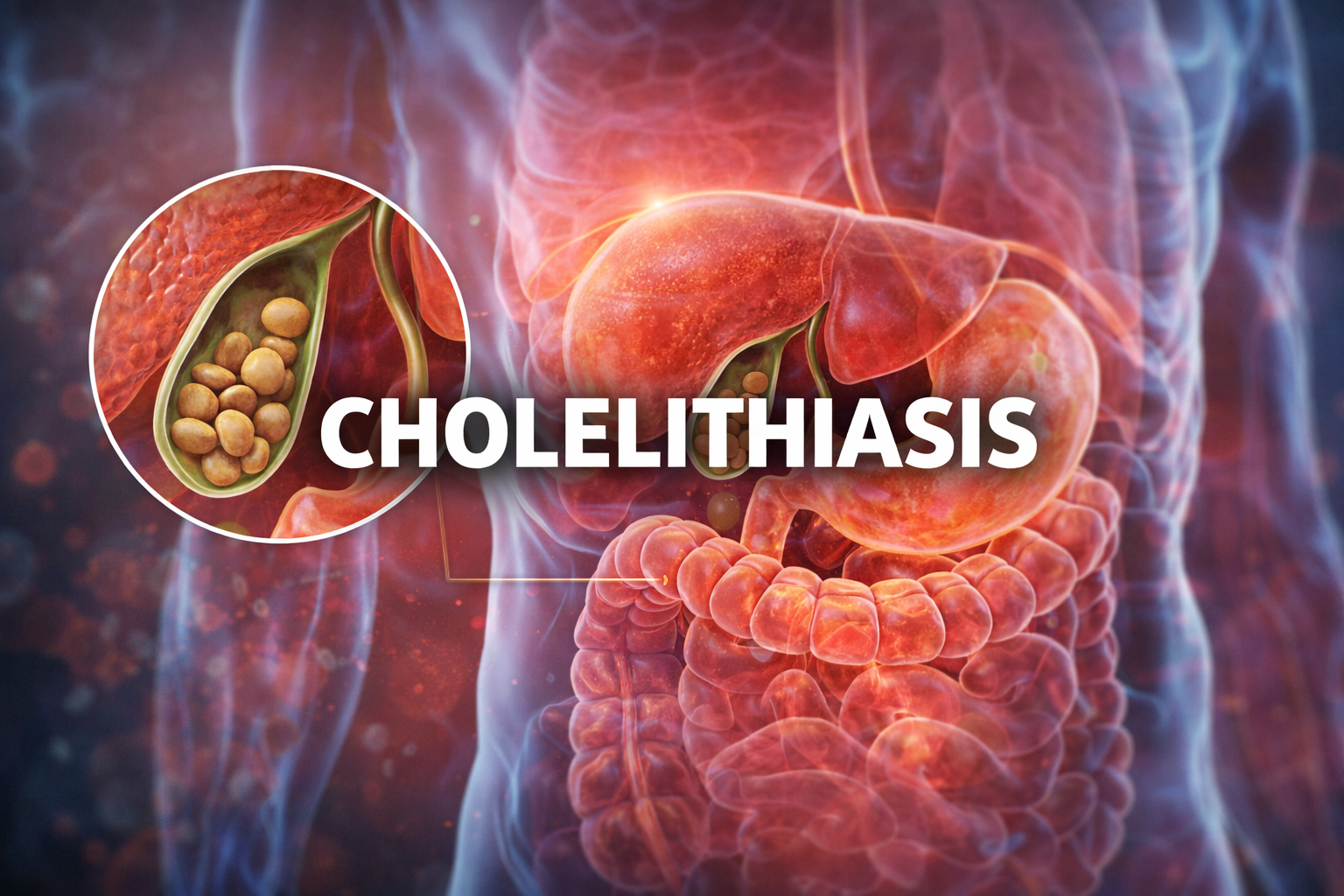
Cholelithiasis
Cholelithiasis—commonly known as gallstones—is one of the most frequently diagnosed digestive conditions worldwide. Despite how common it is, many people don’t fully understand what it means, why it happens, or how it can affect long-term health. Some individuals live their entire lives with gallstones and never notice them, while others experience sudden, intense pain that leads straight to the emergency room.
This article is designed to give you a deep, expert-level understanding of cholelithiasis while keeping the tone approachable and practical. Whether you are researching for personal knowledge, academic purposes, or professional insight, you’ll find everything you need here—from the science behind gallstone formation to modern treatments and prevention strategies.
Let’s begin by understanding exactly what cholelithiasis is and why it matters more than many people realize.
What Is Cholelithiasis?
Cholelithiasis refers to the formation of solid particles—called gallstones—inside the gallbladder. The gallbladder is a small, pear-shaped organ located beneath the liver, responsible for storing bile. Bile is a digestive fluid that helps break down fats, allowing your body to absorb essential nutrients efficiently.
Gallstones form when there is an imbalance in the substances that make up bile. Normally, bile contains cholesterol, bile salts, and bilirubin in the right proportions. When these components fall out of balance—often due to excess cholesterol or reduced bile salts—tiny crystals begin to develop. Over time, these crystals grow larger and become stones.
Many people assume gallstones are rare, but they are actually extremely common. In fact, a significant portion of the adult population develops them at some point, even if symptoms never appear. The silent nature of the condition is one reason it often goes unnoticed until complications arise.
Understanding cholelithiasis is important because it sits at the intersection of digestion, metabolism, and lifestyle. Diet, genetics, hormones, weight changes, and even certain medications can all influence whether gallstones develop.
The Role of the Gallbladder in Digestive Health
To truly understand cholelithiasis, it helps to first appreciate the gallbladder’s role in your digestive system. Although it is not considered an essential organ—you can live without it—it performs a highly efficient supporting function.
The liver continuously produces bile, but digestion does not happen constantly. Instead of letting bile drip endlessly into the intestines, the gallbladder stores it and releases it only when needed, particularly after you eat fatty foods. This targeted release improves digestion and reduces strain on the digestive tract.
When the gallbladder contracts, bile travels through ducts into the small intestine. There, it emulsifies fats, breaking them into smaller particles that digestive enzymes can process more effectively. Without this step, fat digestion becomes less efficient.
However, this storage system can also create problems. If bile sits too long or becomes overly concentrated, the ingredients begin to crystallize. Think of it like sugar forming crystals at the bottom of a supersaturated solution—the same principle applies here.
Once stones form, they may remain harmless or interfere with bile flow. When blockage occurs, pain and inflammation often follow, marking the transition from silent gallstones to symptomatic cholelithiasis.
Types of Gallstones
Not all gallstones are the same. Understanding the different types can help explain why some people develop symptoms while others do not.
Cholesterol Stones
Cholesterol stones are by far the most common type, accounting for the majority of cases. Despite the name, these stones are not composed purely of cholesterol. Instead, they form when bile contains more cholesterol than it can dissolve.
These stones typically appear yellow-green and can vary widely in size. Some are as small as grains of sand, while others can grow as large as a golf ball.
Several factors increase the likelihood of cholesterol stones, including obesity, high-fat diets, rapid weight loss, and hormonal changes—particularly those related to estrogen.
Pigment Stones
Pigment stones are darker and made primarily of bilirubin, a substance produced when red blood cells break down. These stones are less common but often associated with specific medical conditions.
People with liver disease, chronic infections of the bile ducts, or blood disorders that cause rapid red blood cell destruction are more prone to pigment stones.
Unlike cholesterol stones, pigment stones tend to be smaller but more numerous, sometimes forming clusters that complicate treatment.
Mixed Stones
In reality, many gallstones fall into a mixed category, containing varying proportions of cholesterol, bilirubin, and calcium salts. This diversity is why gallstone composition analysis is sometimes performed after surgical removal.
Recognizing the type of stone can help doctors understand underlying causes and recommend lifestyle adjustments to reduce recurrence risk.
How Gallstones Form: The Science Behind Cholelithiasis
Gallstone formation is not a sudden event—it is usually the result of gradual biochemical changes inside the body.
One major trigger is bile supersaturation. When cholesterol levels exceed what bile salts can manage, microscopic crystals appear. These crystals then clump together, forming larger structures.
Another key factor is gallbladder motility. If the gallbladder does not empty efficiently, bile stagnates. This stagnation provides the perfect environment for crystals to grow.
Mucus secretion inside the gallbladder can also accelerate stone formation by acting as a scaffold where particles attach and expand.
Interestingly, inflammation may play a role as well. Some researchers believe that subtle inflammatory changes alter bile composition, further encouraging crystal development.
The process often takes years, which is why gallstones are more common in adults than in younger populations.
Risk Factors You Should Know
Cholelithiasis rarely has a single cause. Instead, it results from a combination of biological and lifestyle influences.
One widely cited memory aid is the “four Fs”: female, forty, fertile, and fat. While somewhat simplistic, it highlights key trends seen in medical research.
Women are more likely to develop gallstones due to hormonal effects that increase cholesterol in bile. Pregnancy and hormone therapy can further elevate risk.
Age is another factor. As people grow older, bile composition changes, and gallbladder efficiency may decline.
Weight plays a surprisingly complex role. Obesity increases cholesterol production, raising gallstone risk. Yet rapid weight loss—especially after bariatric surgery—can also trigger stone formation because the liver secretes extra cholesterol during fat breakdown.
Genetics matter too. If gallstones run in your family, your chances are higher.
Diet, diabetes, sedentary lifestyle, and certain medications round out the list of contributors.
Symptoms of Cholelithiasis
Many individuals with gallstones experience no symptoms at all. These are called “silent stones,” and they often require no treatment.
When symptoms do occur, they typically appear suddenly and can be quite intense.
The most recognizable symptom is biliary colic—a sharp pain in the upper right abdomen. This pain may radiate toward the back or right shoulder blade and often begins after eating a heavy or fatty meal.
Episodes can last anywhere from minutes to several hours. Unlike general stomach aches, biliary colic tends to remain steady rather than coming in waves.
Other symptoms may include:
- Nausea
- Vomiting
- Bloating
- Indigestion
- Intolerance to fatty foods
If a stone blocks a duct for an extended period, more serious symptoms can develop, such as fever, jaundice, or persistent pain. These signs require immediate medical evaluation.
Silent vs. Symptomatic Gallstones
One of the most interesting aspects of cholelithiasis is that not all stones cause trouble.
Silent gallstones are often discovered accidentally during imaging tests performed for unrelated reasons. In most cases, doctors recommend leaving them alone unless symptoms appear.
The logic is simple: surgery carries risks, and many people with silent stones will never experience complications.
Symptomatic gallstones, however, usually demand attention. Once pain begins, episodes often recur and may worsen over time.
Doctors typically evaluate frequency, severity, and risk of complications before recommending treatment.
Understanding this distinction prevents unnecessary anxiety. Having gallstones does not automatically mean you need surgery.
Complications of Untreated Cholelithiasis
Although some gallstones remain harmless, others can lead to serious medical conditions if ignored.
Acute Cholecystitis
This occurs when a stone blocks the cystic duct, causing inflammation of the gallbladder. Symptoms include severe pain, fever, and tenderness in the abdomen.
Without treatment, the gallbladder can become infected or even rupture—both medical emergencies.
Choledocholithiasis
When stones migrate into the common bile duct, bile flow becomes obstructed. This can result in jaundice, dark urine, and pale stools.
Because bile is essential for digestion and toxin removal, blockage must be addressed quickly.
Pancreatitis
In some cases, gallstones block the pancreatic duct, triggering inflammation of the pancreas. Gallstone pancreatitis can range from mild to life-threatening.
Cholangitis
This is a bacterial infection of the bile ducts and requires urgent care. Symptoms often include fever, chills, and confusion.
The takeaway is clear: while gallstones may start quietly, complications can escalate rapidly.
How Cholelithiasis Is Diagnosed
Diagnosis typically begins with a clinical evaluation. Doctors ask about symptoms, pain patterns, and dietary triggers.
The most commonly used imaging tool is ultrasound. It is noninvasive, widely available, and highly effective at detecting stones.
If further detail is needed, additional tests may include CT scans, MRI-based imaging, or specialized procedures that visualize bile ducts more clearly.
Blood tests can reveal signs of infection, inflammation, or bile obstruction.
Early diagnosis allows for better treatment planning and reduces the risk of emergency situations.
Treatment Options for Cholelithiasis
Treatment depends largely on symptom severity.
Watchful Waiting
For silent stones, monitoring is often sufficient. Patients are advised to watch for warning signs while maintaining healthy lifestyle habits.
Medications
Certain drugs can dissolve cholesterol stones, but this approach is slow and not always effective. Stones may return once treatment stops.
Surgical Removal (Cholecystectomy)
The most definitive treatment is removal of the gallbladder. Modern procedures are usually performed laparoscopically, meaning smaller incisions, less pain, and faster recovery.
Most patients return to normal activities within a week.
Importantly, the body adapts well after gallbladder removal. Bile flows directly from the liver into the intestine, allowing digestion to continue with minimal disruption.
Life After Gallbladder Removal
Many people worry that losing the gallbladder will dramatically change their digestion. Fortunately, this is rarely the case.
Initially, some patients notice mild diarrhea or difficulty digesting very fatty foods. These symptoms usually improve as the body adjusts.
Eating smaller, balanced meals helps during recovery.
Long-term, most individuals live completely normal lives without dietary restrictions.
In fact, many feel better than before because the recurring pain is gone.
Dietary Strategies to Reduce Risk
Diet plays a powerful role in gallstone prevention.
A fiber-rich diet supports healthy digestion and helps regulate cholesterol levels. Whole grains, fruits, vegetables, and legumes are excellent choices.
Healthy fats—such as those found in nuts, seeds, and olive oil—can stimulate regular gallbladder emptying, reducing bile stagnation.
Crash diets should be avoided. Gradual weight loss is far safer and less likely to trigger stone formation.
Staying hydrated also supports proper bile consistency.
Rather than focusing on strict rules, aim for sustainable eating habits that promote overall metabolic health.
The Link Between Obesity, Metabolism, and Gallstones
Obesity increases cholesterol secretion into bile, tipping the balance toward crystal formation.
Insulin resistance, commonly associated with metabolic syndrome, may further alter bile chemistry.
Interestingly, fat distribution matters too. Visceral fat—the type stored around abdominal organs—appears particularly influential.
However, the relationship is nuanced. Rapid fat loss can overwhelm the liver with cholesterol, temporarily raising gallstone risk.
This is why medically supervised weight loss programs often include preventive strategies.
Maintaining a stable, healthy weight is one of the most reliable ways to lower risk.
Hormones and Cholelithiasis
Hormonal fluctuations significantly influence gallstone development.
Estrogen increases cholesterol concentration in bile, while progesterone can slow gallbladder contractions.
This explains why gallstones are more common during pregnancy.
Hormonal contraceptives and replacement therapies may also contribute, though modern formulations tend to carry lower risk than older ones.
Understanding this connection allows patients and healthcare providers to make informed decisions when evaluating treatment options.
Genetic and Ethnic Considerations
Genetics can predispose certain individuals to gallstones regardless of lifestyle.
Some populations show higher prevalence due to inherited variations in cholesterol metabolism and bile composition.
Family history should not be ignored during risk assessments.
While you cannot change your genetics, awareness empowers you to adopt preventive habits earlier.
Think of it as managing probability rather than inevitability.
Can Cholelithiasis Be Prevented?
Complete prevention is not always possible, but risk can Cholelithiasis be reduced substantially.
Focus on consistency rather than extremes—steady weight, balanced nutrition, and regular physical activity.
Avoid prolonged fasting unless medically advised.
If you are undergoing rapid weight loss, speak with a healthcare provider about preventive measures.
Small daily choices often have the biggest long-term impact.
Conclusion
Medical science continues to Cholelithiasis explore less invasive ways to manage gallstones.
Researchers are investigating drugs that better regulate bile composition, as well as techniques that break stones apart without surgery.
Advances in imaging are improving early detection, making it easier to intervene Cholelithiasis before complications arise.
There is also growing interest in the gut microbiome’s role in bile metabolism. CholelithiasisFuture therapies may involve microbial modulation to reduce stone formation.
While surgery remains the gold standard today, tomorrow’s treatments may Cholelithiasisoffer more personalized approaches.



